Evidence-Based Decision Making
Gingival Curettage
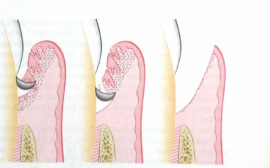
Gingival curettage is one of the three expanded functions of the RDH including anesthesia and nitrous oxide sedation. It is one of the oldest forms of treatment for periodontal pockets however in recent years, there has been a paradigm shift. It is thought that scaling and root planing today, often results in optimal healing without curettage. I chose to do my PICO question on gingival curettage because it is a controversial topic and procedure that I will be preforming during my education.
PICO: Patient/Problem, Intervention, Comparison, Outcome
P: A patient has undergone SRP and has chronically inflamed granulation tissue.
I: Subgingival curettage using hand instruments.
C: Compared with subgingival curettage using a 810-nm 2W diode laser.
O: Promote healing and shrink edematous, enlarged tissue.
Journal Article:
Gingival curettage study comparing a laser treatment to hand instruments
Patient selection for the study included the following:
-18 patients (10 men & 8 women)
-Age range of 25-65 years with a mean age of 40.33 years
-Mild to moderate chronic periodontitis
To be included in the study, patients must meet the following criteria:
-Good overall health indicated by a thorough medical history
-At least 20 natural teeth present (excluding third molars)
-Average plaque level of less than or equal to 1 (Quigley & Hein plaque index)
-Evidence of bleeding and gingivitis
Patients would be excluded from the study for any of the following reasons:
-Presence of a systemic disease
-Current pregnancy/physical condition that limits treatment
-Use of medications that may affect gingival health
-Presence of rampant caries
-Requirement of antibiotic premedication
The study preformed was a single-blind, split-mouth, randomized study. The control group is gingival curettage using hand instruments and the test group is gingival curettage with a 810-nm diode laser using an energy of 2 watts. Each quadrant was randomly choosen to be treated by either the laser or hand instruments. The same operator treated all patients and oral hygiene instructions were given at the initial/baseline visit, as well as following treatment at weeks one and four. During treatment, patients did not have local anesthesia. First, the patients received periodontal debridement with an ultrasonic device. Then, the control group received gingival curettage with the use of hand instruments while the test group received gingival curettage using the Odyssey diode laser set at specific conditions. Following the procedure, the quadrant was irrigated with 1.0% chlorhexidine gluconate solution.
The following assessments were taken on the inital/baseline visit, and at weeks one and four after the completed therapy (by a different qualified examiner, not the therapist):
-Plaque index (PI)
-Gingival index (GI)
-Sulcus Bleeding Index (SBI)
-Pocket Depth (PD)
-Clinical Attachment Level (CAL)
-Visual Analog Scale (VAS)
-Treatment time for each tooth
At baseline there were no major differences between the assessments preformed. The plaque index (PI), gingival index (GI) and bleeding index (SBI) showed a significant improvement for both of the groups when compared to the inital/baseline assessments. Both groups also showed a decrease in pocket depth and increase in clinical attachment level at the four week appointment. While the visual analog scale showed a significant difference between the two groups during treatment, there was no significant differences at the following appointments. Overall, the treatment time was significantly less with the use of a laser when compared to hand instrumentation.
The use of lasers in dentistry are becoming more and more popular. Lasers can be used as an adjunct to scaling and root planing or as an alternative nonsurgical treatment modality since they have been shown to "remove calculus, etch roots and create a biocompatible surface for effective reattachment" (Lin et al, 2011). While some studies suggest that the use of lasers are considered superior to hand scaling, this particular study showed that there were no significant differences at the re-evaluation appointment four weeks later. One difference noted was that patients in the test group (laser assisted therapy) perceived less discomfort during the treatment, however, this too showed no significant difference at weeks one and four following treatment.
In this study, the advantages of using the laser compared to hand instrumentation included increased coagulation, decreased pain, increased patient acceptance, shorter operating time and less effort. On the other hand, lasers are not the preferred method for calculus removal. Conventional non-surgical periodontal therapy includes the use of ultrasonic scalers and hand instruments. It takes a great amount of skill, time and effort to effectively use hand instruments for gingival curettage. Results from this study indicate that the use of the diode laser for curettage can be an effective alternate for periodontal treatment.
Citation:
Lin, J., Bi, L., Wang, L., Song, Y., Ma, W., Jensen, S., & Cao, D. (2011). Gingival curettage study comparing a laser treatment
to hand instruments. Lasers In Medical Science, 26(1), 7-11.
Personal Reflection:
I chose gingival curettage as my topic for this project because is it is an expanded function of the RDH that I will be preforming at some point in my education. I wanted to learn more about this topic since its effectiveness is controversial. I wanted to research alternatives to curettage and found out about the use of lasers and was intrigued by this. Technology is always advancing and there is always the possibility that I will use a laser at some point in my future career. The doctors that I previously worked for had the Waterlase laser and I got to see them use it for various procedures. I feel more knowledgeable about the use of lasers in comparison to hand instruments for curettage procedures after researching this topic and this article.
Additional Information:
The following link takes you to a youtube video on "Wavelength-Optimized Periodontal Therapy".
http://youtu.be/ZNGAAQA2O1w
The following link is to the American Academy of Periodontology (AAP) statement regarding gingival curettage.
http://www.perio.org/resources-products/pdf/38-curettage.pdf
PICO: Patient/Problem, Intervention, Comparison, Outcome
P: A patient has undergone SRP and has chronically inflamed granulation tissue.
I: Subgingival curettage using hand instruments.
C: Compared with subgingival curettage using a 810-nm 2W diode laser.
O: Promote healing and shrink edematous, enlarged tissue.
Journal Article:
Gingival curettage study comparing a laser treatment to hand instruments
Patient selection for the study included the following:
-18 patients (10 men & 8 women)
-Age range of 25-65 years with a mean age of 40.33 years
-Mild to moderate chronic periodontitis
To be included in the study, patients must meet the following criteria:
-Good overall health indicated by a thorough medical history
-At least 20 natural teeth present (excluding third molars)
-Average plaque level of less than or equal to 1 (Quigley & Hein plaque index)
-Evidence of bleeding and gingivitis
Patients would be excluded from the study for any of the following reasons:
-Presence of a systemic disease
-Current pregnancy/physical condition that limits treatment
-Use of medications that may affect gingival health
-Presence of rampant caries
-Requirement of antibiotic premedication
The study preformed was a single-blind, split-mouth, randomized study. The control group is gingival curettage using hand instruments and the test group is gingival curettage with a 810-nm diode laser using an energy of 2 watts. Each quadrant was randomly choosen to be treated by either the laser or hand instruments. The same operator treated all patients and oral hygiene instructions were given at the initial/baseline visit, as well as following treatment at weeks one and four. During treatment, patients did not have local anesthesia. First, the patients received periodontal debridement with an ultrasonic device. Then, the control group received gingival curettage with the use of hand instruments while the test group received gingival curettage using the Odyssey diode laser set at specific conditions. Following the procedure, the quadrant was irrigated with 1.0% chlorhexidine gluconate solution.
The following assessments were taken on the inital/baseline visit, and at weeks one and four after the completed therapy (by a different qualified examiner, not the therapist):
-Plaque index (PI)
-Gingival index (GI)
-Sulcus Bleeding Index (SBI)
-Pocket Depth (PD)
-Clinical Attachment Level (CAL)
-Visual Analog Scale (VAS)
-Treatment time for each tooth
At baseline there were no major differences between the assessments preformed. The plaque index (PI), gingival index (GI) and bleeding index (SBI) showed a significant improvement for both of the groups when compared to the inital/baseline assessments. Both groups also showed a decrease in pocket depth and increase in clinical attachment level at the four week appointment. While the visual analog scale showed a significant difference between the two groups during treatment, there was no significant differences at the following appointments. Overall, the treatment time was significantly less with the use of a laser when compared to hand instrumentation.
The use of lasers in dentistry are becoming more and more popular. Lasers can be used as an adjunct to scaling and root planing or as an alternative nonsurgical treatment modality since they have been shown to "remove calculus, etch roots and create a biocompatible surface for effective reattachment" (Lin et al, 2011). While some studies suggest that the use of lasers are considered superior to hand scaling, this particular study showed that there were no significant differences at the re-evaluation appointment four weeks later. One difference noted was that patients in the test group (laser assisted therapy) perceived less discomfort during the treatment, however, this too showed no significant difference at weeks one and four following treatment.
In this study, the advantages of using the laser compared to hand instrumentation included increased coagulation, decreased pain, increased patient acceptance, shorter operating time and less effort. On the other hand, lasers are not the preferred method for calculus removal. Conventional non-surgical periodontal therapy includes the use of ultrasonic scalers and hand instruments. It takes a great amount of skill, time and effort to effectively use hand instruments for gingival curettage. Results from this study indicate that the use of the diode laser for curettage can be an effective alternate for periodontal treatment.
Citation:
Lin, J., Bi, L., Wang, L., Song, Y., Ma, W., Jensen, S., & Cao, D. (2011). Gingival curettage study comparing a laser treatment
to hand instruments. Lasers In Medical Science, 26(1), 7-11.
Personal Reflection:
I chose gingival curettage as my topic for this project because is it is an expanded function of the RDH that I will be preforming at some point in my education. I wanted to learn more about this topic since its effectiveness is controversial. I wanted to research alternatives to curettage and found out about the use of lasers and was intrigued by this. Technology is always advancing and there is always the possibility that I will use a laser at some point in my future career. The doctors that I previously worked for had the Waterlase laser and I got to see them use it for various procedures. I feel more knowledgeable about the use of lasers in comparison to hand instruments for curettage procedures after researching this topic and this article.
Additional Information:
The following link takes you to a youtube video on "Wavelength-Optimized Periodontal Therapy".
http://youtu.be/ZNGAAQA2O1w
The following link is to the American Academy of Periodontology (AAP) statement regarding gingival curettage.
http://www.perio.org/resources-products/pdf/38-curettage.pdf
**Images retrieved from google.com/images**

